FAQ
Close All | Open All-
What is Root Canal Treatment?
Every tooth has a pulp inside which contains the nerve, blood vessels and connective tissue which is required for the development and immune response of the tooth. Root canal treatment is the removal of the pulp or its remnants, bacteria and necrotic debri within the root canal system by cleaning and shaping the canals, with or without root canal medication and obturation of the root canals by a root filling material.
-
Why Is Root Canal Treatment Necessary?
Root Canal Treatment is necessary when the pulp becomes inflamed or infected due to deep decay, trauma or cracks and the tooth is still restorable or savable. The patient may experience sensitivity to cold or hot, which may be sharp or lingering, or even a toothache that comes on by itself and the tooth may become painful on biting. There may also be a gum swelling or a lump that discharges pus. Sometimes there is no pain at all and a radiolucent lesion is discovered on an xray. Elective root canal treatment is done when the vitality of the pulp is in question and there may be a higher chance of the tooth becoming symptomatic after crowning.
-
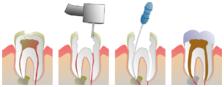
What Is The Root Canal Procedure?
After the tooth is anaesthetised by a local anaesthetic injection, a rubber dam is usually used to isolate the tooth from the rest of the mouth so that saliva does not contaminate the area and root canalirrigants and instruments are contained within the treatment area and visibility is enhanced for the dentist. Decay is removed if any, access is made by drilling to locate the pulp and root canal orifices. Root canal treatment is ideally done under microscopy so that visibility is greatly enhanced and all canals can be located. Ultrasonic tips are used to enlarge the root canal orifices before root canal files are used to negotiate the canals. Very narrow hand files are used initially to create a glidepath for subsequent rotary and/or self adjusting files to be used. Files are used in conjunction with irrigation with various irrigants. The canals are dried with absorbent paper points and may be medicated or root filled with guttapercha that visit or subsequent visit. The access cavity must be filled with a temporary or permanent filling to prevent bacteria from recontaminating the canals.
-
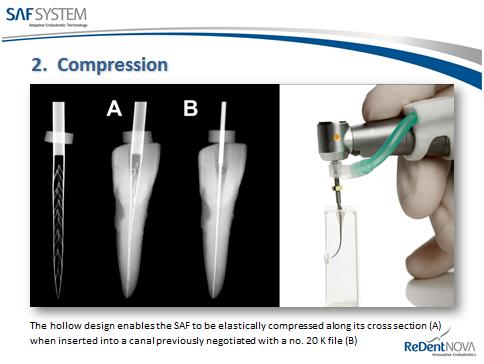
The SAF Self Adjusting File
The SAF is the latest root canal innovation made of flexible nickel titanium that resembles a heart stent mesh that conforms to any root canal shape that has a prior glide path created by smaller hand and rotary files and cleans the canal by means of vertical vibratory scrubbing action(displacement of 0.4mm at 5,000rpm)with a continuous irrigation of irrigant for effective chemo mechanical debridement provided by a peristaltic pump from a vatea irrigation device . So where conventional rotary root canal files which are circular in cross section fail to adequately clean canals of all shapes that are never round in cross section, the SAF is able to increase success rates of root canal treatment.
-
Is Root Canal Treatment Painful?
The patient having root canal treatment should not feel pain if local anaesthesia(LA) is adequately administered. Occasionallly the patient can feel pain if the pulp is severely inflamed because LA anaesthetises at the right pH but the pH in an inflamed pulp may not conducive. In such circumstances, the dentist has to give additional LA or by a different technique. In most cases of root canal treatment after the first visit when the pulp has been removed, the treatment may be painless without LA. In many cases of where the pulp is totally “dead” to begin with, there is also no pain.
-
Will there be pain after treatment?
Perhaps in about half the cases, the patient experiences pain after the root canal procedure, either immediately or the day after , lasting 1-2 days usually, ranging in intensity from a mild discomfort to some pain. Often there is no pain, but tenderness on biting lasting from 3 days to a week.
Patients who brux or clench/grind their teeth often experience more tenderness. Occasionally patients have tenderness lasting a month or so. Patients who brux or have cracked their teeth may experience prolonged tenderness, and occasionally the tooth has to be extracted if even retreating the case doesn’t resolve the symptoms.
Also if root canal treatment fails due to persistent infection the symptoms may persist. When a root canal infection is caught early, ie most of the pulp is vital or alive, the chances of success is about 95%; if there is a periapical lesion(dark radiolucent area around the root apex), the success is 85%. If the case is a retreatment with a periapical lesion, the success drops to 60%. Either the bacteria are resistant to treatment or there are mechanical difficulties preventing access to adequately remove the bacteria.A tooth having a periapical lesion is often without symptoms, so there may be no pain.
-
How many appointments are necessary?
The number of appointments varies from one to few, perhaps 4 or more. If the pulp is vital and the tooth asymptomatic, the case can be completed in a single visit. However, if the time allocated is insufficient , for example the back tooth has 4 canals to treat compared to a front tooth with one canal, the case is completed in 2 visits.
If the patient has pain, the treatment is usually completed in 2 or more visits. At the first visit, the diseased pulp is removed and the canals medicated to allow healing and the tooth is root filled when the inflammation has subsided. When there is no periapical lesion or the lesion is small, and the tooth is asymptomatic on the second visit, the case is usually completed in 2 visits. If there is a larger periapical lesion, the root canals may be medicated for 3 – 6 months. When there is radiographic signs of healing, ie the lesion diminishes, the root canals can be filled.
-
Can I save a cracked tooth?
Yes and no. If the crack is enamel deep, definitely yes. If the crack involves the dentine, but not anywhere near the root canal orifices, yes. If the crack stops close to or at the root canal orifice, perhaps half may survive 5 years or more. If the crack enters the root canal or affects the floor of the pulp chamber, the prognosis is poor and root canal treatment is done when the patient is against having an extraction at that point of time. Usually in addition to starting root canal treatment, the tooth is splinted with an orthodontic band cemented, or a temporary crown is prepared and temporarily cemented to prevent further crack propagation leading to tooth loss.
-
Does the Root Canal Treated tooth require Crowning and followup treatment?
Most of the time yes. Sometimes when remaining tooth structure is adequate in front teeth and the patient doesn’t brux, the access cavity is simply filled after the root canal treatment.
Most of the time, the tooth needs a crown or some form of occlusal coverage to prevent future tooth fracture or further crack propagation for cracked teeth. A tooth that requires root canal treatment is usually one that has deep decay and inclusive of the access cavity, the remaining tooth structure may not be adequately strong to withstand biting forces.
-
How can a previously Root Canal Treated tooth fail?
If root canal treatment was successful because bacteria was adequately removed, the tooth could fail if the patient failed to have followup treatment either by filling or crowning for example. The temporary filling could leak within a short time say after a month and bacteria can gain access to reinfect the root canals despite the root filling, especially if there was no additional safety ‘seal’ like a cement/filling over the root filling. Occasionally the tooth cracks after the patient fails to crown it and if the crack entered the root canal, it would most likely fail. Or perhaps the tooth received a post crown and if the remaining tooth/root structure was weak or inadequate, the root could fracture with time.
Sometimes there may be a periapical lesion that is asymptomatic and if root canal treatment was completed in a single visit or there was no radiographic evidence of healing before root filling, there may be persistence of infection.
-
What treatment options are there when root canal treatment fails?
If previous root canal treatment was done but the radiograph shows that the root fill is inadequate, root canal retreatment is the treatment of choice, success rates are about 80% compared to 70% just by a surgical root canal treatment alone. (This is because 8.5% of apical surgery alone cases begin to show deterioration after 5-7 years when they were initially 97% successful at 1 year.) However, if the tooth received a post crown after the root canal procedure, it would then likely require the surgical root canal procedure as the post presents an obstruction to retreating the canal conventionally. This surgical root canal treatment is called apisectomy or apicoectomy.
Root canal retreatment involves the removal of the previous root filling and the canals are recleaned before root filling. Occasionally there is additional treatment or disassembly required before being able to access the root canals, this involves removing the previous crown, post core or filling.Apisectomy involves surgically exposing the root apex, removing the root tip by sectioning, cleaning the canal at the apical end and root filling from the surgical access.
Should root canal retreatment orapisectomy not be an option, or should apisectomy fail long term, then the affected tooth is extracted and replaced with an implant or bridge or left alone.
-
What are the Costs for Root Canal Treatment?
This depends on case complexity and number of visits, ranging from $600 to perhaps $1800, excluding costs for consultation, diagnostic radiographs, disassembly of the post crown or providing a temporary crown or having to cement an orthodontic band or place a large filling where a temporary filling will not suffice. Front teeth may have 1 or even 2 canals, side teeth or premolars may also have 1 or 2 or even 3 canals and back teeth or molars may have 3 or 4 or even 5 canals, sometimes 2 or even 1 canal. Some canals are short, straight and patent, others are long, curved and calcified. Some require broken root canal instruments to be removed from the canal. Some require long term 3 to 6 months of root canal medication.
-
Many people have exclaimed that Root Canal Treatment is very painful. Is it true?
In the vast majority of root canal treatment cases, root canal work is generally pleasant and quite painless. It is most often done under a local anaesthetic. It is only in the rare case when the initial treatment cause you some discomfort or slight pain, which can be easily overcome subsequently with a suitable anaesthetic technique. It is therefore a fallacy to think that root canal treatment is painful, as it often is no more unpleasant than filling a tooth.
-
Why should I undergo Root Canal Treatment?
The pulp or nerve of a tooth is confined in a chamber and a narrow canal (or canals, in the case of molar teeth). This nerve may be subjected to a host of external detrimental factors such as accidental trauma (such as a fall or a road accident), tooth decay and deep filling. When one or more of these factors cause changes in the health of the nerve which causes pain or discomfort, then root canal treatment is often an alternative to extraction of the tooth.
Also, in many instances, a dead tooth with an associated abscess may be painless and the patient unaware of its presence. The dentist, on discovery of such an abscess, may suggest root canal treatment in preference to an extraction. Just ask yourself, would you prefer to lose a tooth completely or to save it via Root Canal Treatment? -
I’m spending so much time, effort and money to save a dead tooth. Is it worth it?
If, in the dentist's opinion, a tooth is a strategic and useful one, then it certainly is worth the time and expense required for root canal treatment to save that tooth. Extraction may be a faster and more often than not, a vastly cheaper alternative. However, it might not be the best option for the patient. Many a times, an extraction leads to subsequent problems, in the form of teeth over growing, drifting and general instability of the whole dental arch.
-
Is root canal on the molars similar to that on the front teeth?
In general principle, root canal treatment is similar irrespective of the tooth being treated. However, molars and other teeth, which have more than one root, have corresponding multiple nerve canals, which are usually much narrower and curved, compared with the single, wide and straight root canals of the front teeth. Instrumentation and cleaning of these multi-rooted teeth therefore is more difficult and requires more time, skill and equipment.
-
Are dental x-rays necessary during the course of root canal treatment?
Yes definitely, if proper root canal work is to be done. As such treatment is carried out entirely within the root or roots, which are not directly visible, guess work has no place in this field.
X-ray may be required before and after treatment, but is certainly required during treatment, as the dentist has to know the exact length of the tooth he is treating as well as the number of roots and the size and shape of the roots canals. -
After the first visit, when the pain has disappeared, can I just leave the root unfilled since it is not bothering me?
No, an unfilled root canal or canals, which may have been cleaned, is only treatment half done. The unfilled root canal predisposes to re-infection or a worsening of the condition of tooth and will definitely cause problems sooner or later. This is because seepage of fluids from the surrounding tissues into the unfilled root canal results in stagnation.
This fluid will eventually breakdown producing irritating by-products that prevent healing of the surrounding tissues. It is therefore important that you have the tooth root filled completely, even if it entails several visits to your dentist. -
After a tooth has been root filled, with its nerve taken out, does it mean that I shall no longer feel any more pain from that tooth?
As the tooth no longer has a nerve supply within itself, you will not feel any pain or sensitivity from that tooth to such stimuli as cold, heat, sweet and sour. However, do not forget that the tooth is still supported by tissue and bone, which are very much alive. Hence, any infection of these supporting tissues will still enable you to feel pain or discomfort to such stimulus as pressure from touching or biting. In addition, infection of the gums surrounding that the tooth will also lead to a painful and sore tooth.
-
Will it be just as strong as my other teeth and can it decay just as my other teeth can?
If your root filled tooth has been well restored or filled or better still crowned, then it certainly will be as strong as other teeth in your mouth. It can and should function also as well as any normal live tooth but unfortunately can also decay just as any tooth can. Of course, there will not be the initial sensitivity or pain as the decay progress, the absence of which may be misleading. It will therefore be just as important to maintain and treat non-vital teeth as you would your other teeth, as these teeth have a vital role to play in your mouth.
-
How much does root canal treatment cost?
The fees vary with the nature of the tooth and the complexity of the case. It may vary from about $200 for a simple front tooth to about $800 for a molar or back tooth. Please call us at 62350646 to arrange for a dental appointment with our dental surgeons. Alternatively, you may request for an appointment here.
1 Grange Rd #10-01 Orchard Building
Singapore 239693
(Located opposite Cineleisure @ Orchard Road)
